Better Access to Mental Health Care
The Federal Government introduced Mental Health Medicare Items on 1 November 2006 that enabled greater access to Psychologists and psychological support services for all Australians.
Every Australian is eligible for a new or renewed Mental Health Care Plan [a GP referral] each Calendar Year that is from 1 January to 31 December annually. A valid and current GP referral is required to claim the medicare rebate.
Click on the link below for more information from Medicare regarding MBS Items covered and the referral process.
FOCUSSED PSYCHOLOGICAL STRATEGIES – ATTRACTING MEDICARE REBATES EACH CALENDAR YEAR
This link provides information on the GP MENTAL HEALTH CARE TREATMENT MBS ITEMS 2700, 2701, 2712, 2713, 2715 and 2717 and includes an overview of the items, patient and provider eligibility, what activities are involved in providing services rebated by these items, links to other Medicare items and additional claiming information.
Here are a list of common concerns and issues raised by GPs when considering referring to a Psychologist.
Do you Bulk Bill?
Many GPs ask us this question. The answer is NO. We do not recommend Bulk Billing for psychological services.
We have provided bulk billing for a small percentage of patients [10% of referrals] with a GP recommendation in the past but we DO NOT RECOMMEND bulk billing because we have found it undermines the process of treatment and sets up a patient to fail.
We find patients who contribute, even a small amount, to the fee receive a significant increase in benefits from treatment. Patients paying for sessions are more motivated to participate in treatment, more likely to follow treatment plans and as a result they are more likely to improve.
We also find that patients not contributing to the fee are extremely likely to cancel or not attend their appointments. For these reasons we strongly discourage offering bulk billing to patients.
How much would my patient be out of pocket?
Out of Pocket Costs
- Full Fee+………………………………………………………………………………………………$100.00
+Until 1 September 2016 we were offering offering some concession rates to 10% of the people we were working with at any one time. We have found providing counselling at a concession rate is associated with a reduction in active participation and commitment, an increase in frequency of cancellations and a corresponding reduction in the positive therapeutic benefits facilitated by counselling. We are no longer offering concession rates for sessions due to these reasons.
How do I discuss the need for psychological treatment with my patient?
Psychological conditions and symptoms, particularly in the case of trauma, are very often many years in the making. It is common for patients to keep their symptoms secret for a long time before attempting to find help. Asking for help can be a confronting experience. Many do not want others to see them as being less or broken in some way. This fear can become a serious obstacle to seeking treatment. There is a risk of humiliation, embarrassment, rejection, shame and or being disbelieved when sharing their experience of symptoms with their GP.
For most patients improvement and symptom reduction is not immediate. This can be disappointing and frustrating for patient, GP and Psychologist. The special trust patients have in their GP can be a powerful way to significantly improving outcomes.
GPs are able to;
- provide an initial safe opportunity for patients to discuss the difficult nature of psychological symptoms
- assist patients by clarifying expectations they may have of psychological treatment
- provide needed motivation and focus when the treatment becomes challenging as it inevitably does
What can I do to improve treatment outcomes for my patient?
We find assisting patients to develop an accurate understanding of the process of psychological treatment, change and recovery assists greatly in achieving good outcomes. We have gathered together a small sample of statements and questions GPs have used with good effect when discussing the need for psychological treatment with their patients;
Q. “How long will it take?”
A. “These symptoms have taken time to develop so they will take time to resolve”
Q. “How can Psychologists help me?”
A. “Psychologists work with the way in which people learn. They help people find new ways to deal with old problems.”
Statement: “I have tried Psychologists before, my situation is too hard. Psychologists can’t help me.”
A. “Many people need to try treatment several times before their symptoms start to improve. Psychology can work for you because it has worked for others. People find the more they can put in to treatment, the quicker their symptoms start to improve. I think we should try again.”
How can I determine when my patient is ready to begin treatment?
Deciding when to offer psychological treatment to a patient is a significant factor in achieving positive outcomes. Not all patients experiencing symptoms are ready to commit to treatment. We have found offering psychological treatment before a patient is ready actually prevents them from accessing treatment and therefore resolving symptoms in the future.
The RACGP recommends using the STAGES OF CHANGE to assist in determining when to offer psychological treatment to a patient.
We have found the Transtheoretical Model of Behaviour Change (Stages of Change) initially developed by Prochaska and DiClemente (1982, 1986) to be a quick, useful, easy to use method of assessing patient readiness to change. This approach is supported by several decades of research across a wide variety of behaviour change in the health care setting.
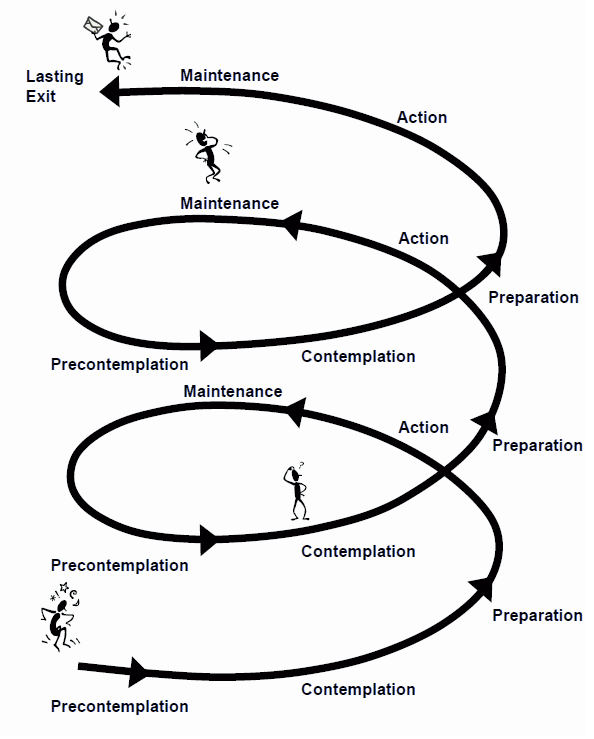
The five stages of change
Precontemplation
People in this stage are not thinking seriously about changing and tend to defend their current thinking and doing patterns. They may not be able to see or be open to examining the role they are playing in their situation. The positives or benefits, of their current approach outweigh any costs or adverse consequences so they are happy to continue on as they are.
Contemplation
People in this stage are able to consider the possibility of examining their thinking and doing patterns but feel ambivalent about taking the next step. On the one hand there are benefits to the way they are currently handling their situation. On the other hand, they are starting to experience some adverse consequences (which may include personal, psychological, physical, legal, social or family problems).
Preparation
Have usually made a recent attempt to change their thinking and doing habits in the last year. Sees the ‘cons’ of continuing as outweighing the ‘pros’ and they are less ambivalent about taking the next step. They are usually taking some small steps towards changing behaviour. They believe that change is necessary and that the time for change is imminent. Equally, some people at this stage decide not to do anything about their behaviour.
Action
Actively involved in taking steps to change thinking and doing habits and making great steps towards significant change. Ambivalence is still very likely at this stage. May try several different techniques and are also at greatest risk of relapse.
Maintenance
Able to successfully avoid any temptations to return to return to previous thinking and doing habits. They have learned to anticipate and handle challenges and are able to employ new ways of coping. They can have a temporary slips and challenges to sustaining change but don’t tend to see this as failure.
“CHANGE ~ READY OR NOT?”
What ‘Stage of Change’ is your patient currently experiencing?
NOT READY FOR CHANGE
If your patient is not ready to change, that is, they are in PRECONTEMPLATION or RELAPSE we recommend;
- Validating their current position
- Providing information
- Providing contact details for Telephone Counselling Service contact details such as Life Line 13 11 14
READY FOR CHANGE
If your patient is considering making change, that is, they are in CONTEMPLATION or PREPARATION, we recommend;
- Assisting the patient to identify the negative impact their symptoms are having on their quality of life
- Introducing and offering psychological treatment as a way forward